|
8/24/2023 0 Comments Gram negative rods in csf
WBC 471/mm 3, protein 55 mg/dL, glucose 25 mg/dL/ Ventricular fluid and peritoneal catheter cultures with Listeria monocytogenes, quantitative real- time PCR for hly geneĭay 7: ventricular catheter removal and EVD placement WBC 480/mm 3, protein 46 mg/dL, glucose 35 mg/dL/ĬSF and ascites fluid cultures with Listeria innocua At the follow-up appointment 10 days after hospital discharge and after completion of his antibiotic course, he had no residual symptoms. Due to rapid sterilization of cultures after initiation of ampicillin and clinical improvement, we did not initiate intraventricular antibiotics. He received a total of 3 weeks of parenteral ampicillin. After 7 days of therapy, we placed a new VPS on the left side. We discontinued vancomycin and ceftriaxone and removed the entire right-sided VPS, with temporary placement of an external ventricular drain (EVD). Susceptibility testing was performed using the MicroScan Pos Combo 33 Panel and interpreted with CLSI M45-A2 guidelines, which demonstrated that both isolates were susceptible to ampicillin and penicillin. monocytogenes on blood and chocolate agar plates within 24 hours. The ventricular and abdominal pseudocyst fluid cultures grew L. We observed short Gram-positive rods in the CSF ( Figure 2), and added ampicillin 75 mg/kg every 6 hours to the regimen. A blood culture was not obtained prior to initiating antibiotics. He was empirically treated with parenteral vancomycin 20 mg/kg every 8 hours and ceftriaxone 100 mg/kg every 24 hours. A lumbar aspiration was not performed.Ībdominal ultrasound showing CSF pseudocyst. 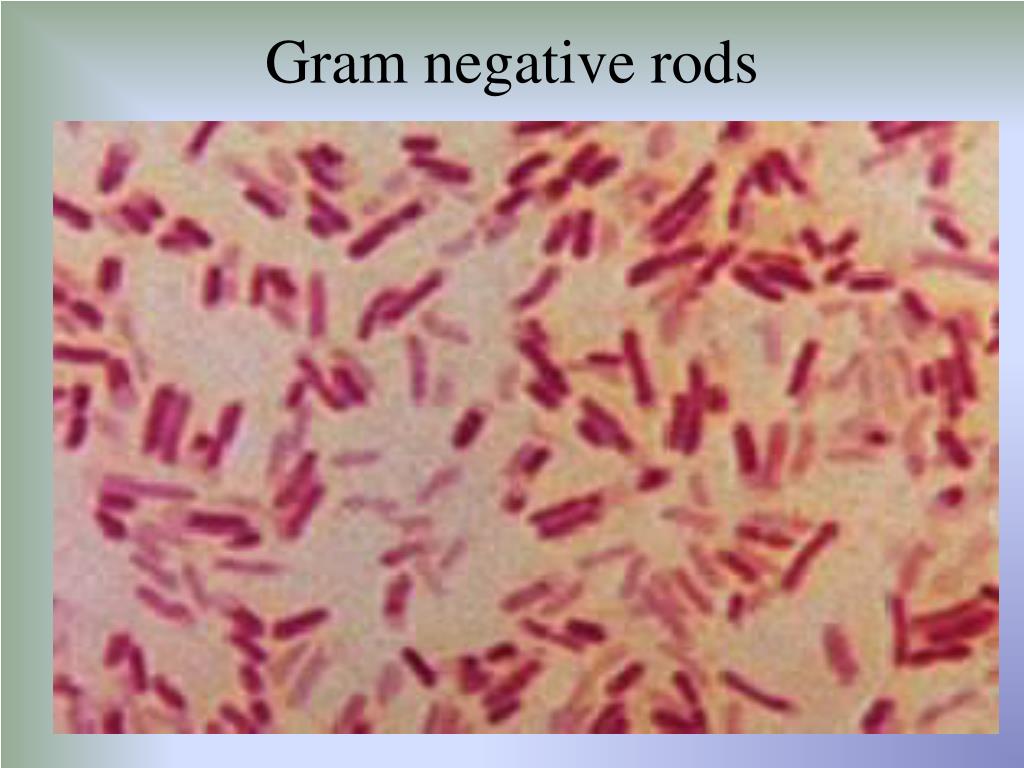
His ventricular fluid glucose was 37 mg/dL, and his protein was 60 mg/dL. His ventricular fluid was straw colored, with a leukocyte count elevated to 585/UL with 23.3% neutrophils, 28% lymphocytes, 45% monocytes/macrophages, and 3.7% atypical/reactive lymphocytes. We externalized the lower portion of his VPS, drained the pseudocyst, and sent the fluid for culture. Computed tomography of the head showed stable ventriculomegaly compared with previous imaging. Abdominal ultrasound revealed a large, multiloculated, septated cystic lesion encompassing part of the shunt catheter including the tip, consistent with a CSF pseudocyst ( Figure 1). His C-reactive protein was elevated at 18.1 mg/dL. He had hyponatremia (129 mmol/L) and hypoalbuminemia (2.8 mg/dL), but the rest of his complete metabolic panel was unremarkable. His peripheral leukocyte count was 7.2 thou/mL, his hemoglobin was 11.8 g/dL, and his platelet count was 637 thou/mL. He had a diffusely tender abdomen with distension, hypoactive bowel sounds, and guarding on examination. He did not ingest unpasteurized milk or cheese, cold cuts, or raw or undercooked meat, but he ate vegetables from the local supermarket. The family denied any local or foreign travel since immigrating to the United States, foreign visitors, or animal exposures. Similarly, his CD19+ B (597 cells/uL) and NK cells (260 cells/uL) were within normal limits. His CD4+ and CD8+ T-cell counts were within normal limits for his age, at 1203 cells/uL and 643 cells/uL, respectively. His immunizations were up to date without associated adverse reactions, and he tested negative for human immunodeficiency virus. He was diagnosed with pulmonary tuberculosis at 20 months of age and treated, under direct observation, with rifampin, isoniazid, pyrazinamide, ethambutol (RIPE) and pyridoxine. He migrated to the United States at 19 months of age. A right-sided VPS was placed at 8 months of age without subsequent revisions or access. His medical history was significant for communicating hydrocephalus diagnosed at 4 months of age in Uganda, where he was born to parents who were refugees from the Democratic Republic of Congo. He presented to our emergency department after having 2 days of progressively worsening abdominal distension and pain. Over the following week, he clinically improved but his appetite remained poor. Two weeks before presentation, he had been ill with nonbloody, nonbilious vomiting for 1 day and tactile fever for 4 days. A 3-year-old male with a history of VP shunt (VPS)–dependent hydrocephalus of unknown etiology presented with fever and abdominal distension.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
